Effect of Anxiety and Depression on Survival of Cancer Patients, a 13 Year Follow-up
Download
Abstract
Introduction: Anxiety and depression occur at a high rate in cancer patients. However, debate remains regarding the effect of anxiety and depression on cancer survival.
Objective: This study aimed to determine the effect of anxiety and depressive symptoms on the survival of cancer patients.
Methods: The subjects consisted of 112 cancer patients who attended the Oncology and Radiotherapy outpatient clinic Hospital Kuala Lumpur, Malaysia, in 1999. Anxiety and depressive symptoms were measured using the Hospital Anxiety and Depression Scale (HADS) questionnaire at inception. Information on patients’ mortality status for extended 13 years follow-up (in 2011) was obtained from the National Registration Department death records. Overall survival for each anxiety and depressive symptoms scores in HADS at 13 years was calculated using Cox proportional hazards regression analysis. Results: Cancer patients experienced more anxiety (83%) compared to depressive symptoms (40.2%). The mean (S.D.) HADS scores for depressive symptoms were 9.9 (2.5), and the anxiety symptoms score was 12.6 (2.1). At 13 years, half of the patients (50.9%) had died. No significant effect of anxiety (p=0.399, 95% C.I.= 6.2-8.4) or depressive symptoms at inception (p=0.749, 95% C.I.= 5.9-8.4) towards cancer patients’ survival was found at 13 years follow-up.
Conclusion: The occurrence of anxiety symptoms among cancer patients in this study was 2-folds higher than depressive symptoms. However, no significant increased risk of death was found in cancer patients with anxiety or depressive symptoms at 13 years follow-up. It may imply that as time extended, survival in cancer patients may be related to various interacting elements, and intervening health factors are of importance.
Introduction
The prevalence of depression among cancer patients ranged between 8% to 24% and differed by the type of instruments used in the study, type of cancer, and treatment phase [1]. Meanwhile, the prevalence of anxiety disorders among cancer patients ranged between 17-26%) [2]. Most patients have subthreshold symptoms or subsyndromal without meeting diagnostic criteria [3]. However, past research into the role of psychological factors in cancer survival has yielded mixed results.
A study by Watson et al. [4] showed significantly increased risk of death by five years in women with a high score on depression subscale but not with anxiety. At 17 years of follow-up, Shekelle et al. [5] reported a 2-folds higher mortality rate in depressed cancer patients. In a prospective study of patients diagnosed with hepatobiliary cancer, Steel et al. [6] found that depression affects their survival times. This study showed that depression occurs in over one-third of the patients, and these patients have a substantially reduced survival period, particularly among patients with evidence of tumour vascular invasion [6]. In contrast, some studies have shown that depression does not affect cancer mortality [7-8].
A meta-analysis found evidence that depression predicted mortality in cancer patients, but not progression [9]. The associated risk is statistically significant but relatively small [9]. The impact of depression persist even after clinical predictors had been adjusted, indicating that depression may play a causal role. Endocrinological and immunological pathways have been suggested to explain the relationship between distress and survival in cancer patients [9-11].
To date, only a few studies have looked at survival in cancer patients longer than ten years. Longitudinal study designs could track effects of psychological distress towards cancer survival and progression, both short-term and long-term, following cancer diagnosis [12]. The present study aimed to examine the effects of anxiety and depressive symptoms on cancer patients’ survival in Malaysia. Survival status was assessed at 13 years after initial recruitment. We hypothesised that anxiety or depressive symptoms are associated with lower survival in cancer patients.
Materials and Methods
Study design
Subjects were recruited in 1999 if they met the following criteria: i) cancer diagnosis ii) 18 years or older iii) able to speak or read in Malay or English iv) able to give informed consent. The study was conducted in the Oncology and Radiotherapy outpatient clinic, Hospital Kuala Lumpur, Malaysia.
At the study entry, the following information was collected: age, gender, ethnicity, marital status, education, diagnosis, cancer stage, and treatment modalities. Each participant completed the Hospital Anxiety and Depression Scale (HADS) questionnaire. HADS is an established screening instrument for detecting anxiety and depressive symptoms in cancer patients.
Consent was obtained during subjects’ recruitment. Anxiety and depressive symptoms were assessed using the Hospital Anxiety and Depression Scale (HADS) questionnaire (HADS) [13]. Data on mortality status of patients was collected from the death records of the National Registration Department for the extended 13 years follow-up (in 2011).
Study Instruments
Participants’ depressive and anxiety symptoms were assessed using the Hospital Anxiety and Depression Scale (HADS) [13]. HADS is an established anxiety and depression screening tool for patients with cancer.
HADS consists of 14 questions; seven items assess anxiety symptoms (HADS-A) and seven items for depressive symptoms (HADS-D). The items were scored from zero (not present) to three (considerable) on a four-point scale.
HADS-D includes 1, 3, 5, 7, 9, 10, 13, and HADS-A contains items 2, 4, 6, 8, 11, 12, 14. Each item score was summed, giving sub-scale scores on the HADS-A and the HADS-D from zero to 21. For each subscale, scores from 0-7 were categorised as “no problem,” 8 to 10 “mild symptom,” 12 to 14 “moderate cases,” and scores above 15 as “severe symptom.” In brief, any domain score ≥ 8 was considered a “case.”
Statistical analysis
Descriptive analysis, such as the frequency with percentage and mean with standard deviation, were used to present the demographic profile of respondents and the status of psychological symptoms. Kaplan – Meier with a log-rank test was used to determine the survival time over 13 years follow up and whether the state of anxiety and depression does affect the survival time. All analyses were carried out using SPSS (SPSS Inc. Released 2009. PASW Statistics for Windows, Version 18.0. Chicago: SPSS Inc).
Results
Socio-demographic profile of participants
Table 1 shows the socio-demographic profile of the participants. The subjects consisted of 112 cancer patients who attended the Radiotherapy and Oncology outpatient clinic, Hospital Kuala Lumpur, Malaysia, in 1999. The mean (S.D.) age of participants was 61.9 (13.0) years. Women are over-represented (65.2%). Most of them were Malays (61.6%) and married (74.1%). Almost half of them had an educational level up to secondary school (42%).
| Profile | Mean (S.D.) | Frequency (percent) |
| Age | 61.9 (13.6) | |
| Gender | ||
| Male | 39 (34.8) | |
| Female | 73 (65.2) | |
| Ethnicity | ||
| Malay | 69 (61.6) | |
| Chinese | 19 (17.0) | |
| Indian | 18 (16.1) | |
| Others | 6 (5.4) | |
| Marital status | ||
| Single | 9 (8.0) | |
| Married | 83 (74.1) | |
| Widow/widower | 12 (10.7) | |
| Divorced | 8 (7.1) | |
| Education | ||
| None | 18 (16.1) | |
| Primary | 35 (31.3) | |
| Secondary | 47 (42.0) | |
| Tertiary | 7 (6.3) | |
| No record | 5 (4.5) |
Cancer types were mixed with the majority of patients diagnosed with breast cancer (23.2.%), followed by cancer involving head or neck area (22.3%), cancer of reproductive system (14.3%), respiratory system (6.3%), gastrointestinal system (6.3%), and others (27.6%). More than half of the participants (50.9%) were in the late stages of cancer (stage III and IV), 25.9% in stage II, and 9.8% in stage I.
Survival Patterns of Cancer Patients and Its Association with Anxiety And Depressive Symptoms
Table 2 demonstrated that more cancer patients experienced anxiety (49.1%) compared to depressive symptoms (6.3%). About 33.3% of patients experienced mixed anxiety and depressive symptoms.
| Status | N | % |
| None | 12 | 10.7 |
| Depression | 7 | 6.3 |
| Anxiety | 55 | 49.1 |
| Depression and anxiety | 38 | 33.9 |
The mean HADS score for anxiety symptoms was higher (12.6) than depressive symptoms (9.9). After 13 years, a total of 55 participants (49.1%) were still alive, and 57 (50.9%) had died. Kaplan Meier cumulative curves evaluated at 13 years (Figure 1) showed a tendency for lower survival for patients who had depression at baseline compared to those with anxiety alone or mixed symptoms.
Figure 1. Survival Function of Cancer Patients at 13 years.
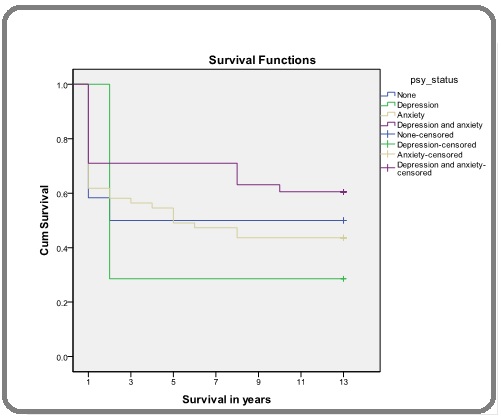
However, depression, anxiety, or mixed symptoms did not affect cancer survival (p=0.538), and even after controlling for cancer stage (p=0.187) (Table 3).
| Status | Mean (years) | S.E. | 95%CI | median | S.E. | 95% C.I | ||
| None | 6.8 | 1.8 | 3.3 | 10.3 | 2 | . | . | . |
| Depression | 4 | 2.2 | 0 | 8.2 | 0 | . | . | . |
| Anxiety | 6.6 | 0.8 | 5.1 | 8.2 | 5 | 2.6 | 0 | 10.2 |
| Both | 8.9 | 0.9 | 7.1 | 10.7 | . | . | . | . |
| Overall | 7.3 | 0.6 | 6.1 | 8.4 | 8 | . | . | . |
Note, P – value from Log Rank (Mantel-Cox) test, 0.187
Discussions
Contrary to our hypothesis, this study did not find an association between anxiety, depression, or mixed symptoms with cancer survival at 13 years follow- up. A meta-analysis found that depression-mortality correlations were highest in intervals of less than two years and concluded that, as the survival time prolonged, other intervening factors were more likely to account for mortality [14]. The severity of anxiety and depressive symptoms may change over time; hence, the scores of anxiety and depressive symptoms at the study baseline may lose predictive power as the correlative stability decreases with increasing study intervals [15]. Furthermore, prospective studies that found no correlation between depression and cancer progression had an average period of ten years [11]. Satin et al. [9] reported that the results of studies with longer duration were inconclusive. Biological functions may have a more significant role affecting cancer progression, and mortality as more than half of the patients in this study was in advanced cancer stage [16]. In Malaysia, although there are established and accessible cancer screening programmes for breast, cervix uteri and colorectal cancers, the percentage of cases who were presented at late stage (stage III and IV) were 41.3%, 38.5% and 63.8%, respectively. Thus, there is a need to strengthened the awareness of cancer prevention in community [17].
Almost half of the patients in this study reported anxiety symptoms, while one-third experienced mixed anxiety and depressive symptoms. Likewise, a local study by Lin et al. [18] also found a higher prevalence of anxiety among cancer patients compared to depression. Anxiety is a response to a threat. One plausible reason is that most patients were already in advanced cancer stages at the time of recruitment. Cancer is a threatening condition for those who are diagnosed with the disease. For some patients, they may be scared of unwelcome side- effects of treatment and physical effects of cancer [19], increased pain, anticipatory grief, and fear of impending death or existential anguish [20]. It is noteworthy that patients with anxiety showed a tendency for better survival than patients with depressive symptoms after 13 years in this study, although the association was insignificant. A meta-analysis by DiMatteo et al. [21] showed a significant and substantial relationship between depression and non-compliance in cancer patients, with an odds ratio of 3.03 (95% confidence interval, 1.96- 4.89); while the association between anxiety with non-compliance were insignificant. There is a possibility that anxiety may have no direct effect on treatment adherence but improve treatment adherence activities in a patient who is anxious about his/her health condition.
There are several limitations in the present study. Firstly, heterogeneity in disease site, status, and prognosis within the sample may lead to potentially different cancer prognosis and psychological consequences. Secondly, the conclusion is constrained using a screening tool without diagnostic specificity. Finally, some important mediators were not tested due to lack of sufficient data (e.g., cancer treatment, comorbidity, the time interval between cancer diagnosis and assessment of psychological distress). Directions for future distress-survival research should focus on site-specific association and include more confounding medical variables such as comorbidities and distinction between curative versus palliative treatment. In conclusion, this present study did not support the hypothesis that anxiety or depressive symptoms were associated with lower survival after 13 years. This may imply that with extended follow-up, survival in cancer patients may be more related to factors other than anxiety or depression. As most cancer patients suffer from anxiety and depressive symptoms, we advocate early psychological screening to initiate therapeutic intervention and psychological support earlier during the disease.
Acknowledgements
This research obtained ethical approval from UKM Research Ethics Committee and was funded by the UKM Young Investigator Grant (GGPM-2012-087). The National Research Register (NMRR) identification number for this research is NMRR-13-1672-15474.
References
- Prevalence of depression in cancer patients: a meta‐analysis of diagnostic interviews and self‐report instruments Krebber A. M. H., Buffart L. M., Kleijn G., Riepma I. C., Bree R., Leemans C. R., Becker A., Brug J., Straten A., Cuijpers P., Verdonck‐de Leeuw I. M.. Psycho-Oncology.2013;23(2). CrossRef
- Psychological effects of being offered choice of surgery for breast cancer Fallowfield L J, Hall A, Maguire P, Baum M, A'Hern R P. BMJ.1994;309(6952). CrossRef
- Depressive symptoms and quality of life in home-care-assisted cancer patients Grassi Luigi, Indelli Monica, Marzola Marina, Maestri Antonio, Santini Alessandra, Piva Erick, Boccalon Massimo. Journal of Pain and Symptom Management.1996;12(5). CrossRef
- Influence of psychological response on survival in breast cancer: a population-based cohort study Watson M, Haviland JS, Greer S, Davidson J, Bliss JM. The Lancet.1999;354(9187). CrossRef
- Psychological Depression and 17-Year Risk of Death from Cancer1 Shekelle Richard B., Raynor William J., Ostfeld Adrian M., Garron David C., Bieliauskas Linas A., Liu Shuguey C., Maliza Carol, Paul Oglesby. Psychosomatic Medicine.1981;43(2). CrossRef
- Depression, Immunity, and Survival in Patients With Hepatobiliary Carcinoma Steel Jennifer L., Geller David A., Gamblin T. Clark, Olek Marion C., Carr Brian I.. Journal of Clinical Oncology.2007;25(17). CrossRef
- Depression as a risk for cancer morbidity and mortality in a nationally representative sample Zonderman AB, Costa PT, McCrae RR. JAMA.1989;262(9):1191-1195.
- Psychosocial morbidity and survival in adult bone marrow transplant recipients--a follow-up study Murphy K, Jenkins P, Whittaker J. Bone Marrow Transplant.1996;18(1):199-201.
- Depression as a predictor of disease progression and mortality in cancer patients Satin Jillian R., Linden Wolfgang, Phillips Melanie J.. Cancer.2009;115(22). CrossRef
- Relation between depression and circulating immune products in patients with advanced colorectal cancer Allen-Mersh T G, Glover Clare, Fordy Carol, Henderson D C, Davies M. Journal of the Royal Society of Medicine.1998;91(8). CrossRef
- Depression and cancer: mechanisms and disease progression Spiegel David, Giese-Davis Janine. Biological Psychiatry.2003;54(3). CrossRef
- Psychological Distress and Cancer Survival Brown Kirk W., Levy Adrian R., Rosberger Zeev, Edgar Linda. Psychosomatic Medicine.2003;65(4). CrossRef
- The Hospital Anxiety and Depression Scale Zigmond A. S., Snaith R. P.. Acta Psychiatrica Scandinavica.1983;67(6). CrossRef
- Depression and cancer mortality: a meta-analysis Pinquart M., Duberstein P. R.. Psychological Medicine.2010;40(11). CrossRef
- Long-term stability of depression, anxiety, and stress syndromes. Lovibond Peter F.. Journal of Abnormal Psychology.1998;107(3). CrossRef
- Psychosocial Factors That Affect the Survival of Adult Cancer Patients Cwikel Julie G., Behar Lynn C., Zabora James R.. Journal of Psychosocial Oncology.1998;15(3-4). CrossRef
- National Cancer Registry Ministry of Health Malaysia. Malaysian Study On Cancer Survival (MySCan). 20182018 .
- Anxiety and depressive symptoms and health-related quality of life status among patients with cancer in Terengganu, Malaysia Lin LP, Yee WS, Selamat NW. ASEAN J of Psychiatry.2011;12(1):18-24.
- Mastering tasks of adolescence: The key to optimum end-of-life care of an adolescent dying of cancer Saini SM, Koon Tan SM. ASEAN J of Psychiatry.2011;12(1 (Jan-June)):126-128.
- Psychological distress in cancer from survivorship to end of life care: Prevalence, associated factors and clinical implications Gao Wei, Bennett Michael I., Stark Daniel, Murray Scott, Higginson Irene J.. European Journal of Cancer.2010;46(11). CrossRef
- Depression Is a Risk Factor for Noncompliance With Medical Treatment DiMatteo M. Robin, Lepper Heidi S., Croghan Thomas W.. Archives of Internal Medicine.2000;160(14). CrossRef
License

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright
© Asian Pacific Journal of Cancer Care , 2021
Author Details
How to Cite
- Abstract viewed - 0 times
- PDF (FULL TEXT) downloaded - 0 times
- Xml downloaded - 0 times