Triple Primary Head and Neck Cancer : A Case Report and Literature Review
Download
Abstract
Globally, head and neck cancer is estimated to occur in more than 700,000 patients a year and cause 400,000 deaths and second most common cancer in India among both sexes and all ages. Even after optimal treatment for primary cancer, there are cases where second primary cancers develop around the previously treated areas. This occurrence is explained by the concept of field cancerization, which refers to a term where a carcinogen such as tobacco when chewed, exposes the mucosa to the carcinogen starting from the oral cavity to the upper aerodigestive tract. Combinations of two primary malignancies are seen in around 3% to 5% of patients, combinations of three cancers in about 0.5%, and combinations of four malignant tumors in about 0.3% of patients with a previous history of cancer. Early diagnosis and detection of these cancers are necessary for optimal treatment as with each occurrence the tolerability and the response rates gets poorer.
Introduction
Globally, head and neck cancer is estimated to occur in more than 700,000 patients a year and cause 400,000 deaths [1]. According to the GLOBOCAN 2020 factsheet, head and neck cancers are the second most common cancer in India among both sexes and all ages with 135,929 (10.3%) of new cases and ranks third for death toll with 75,290 (8.8%) cases. The 5-year prevalence for all ages is 21.77 per 100,000 [2]. Even after optimal treatment for pri-mary cancer, there are cases where second primary cancer developed within the field of primary cancer after more than six months. Field cancerization refers to a term where a carcinogen such as tobacco when chewed, involves a pathway starting from the oral cavity to the upper aero-digestive tract, which may show premalignant lesions and later develop into a frank malignancy. At the cellular level, field cancerization is a growth of mutant cells that creates a field of cells predisposed to subsequent tumor growth [3,4]. Patients with pre-vious head and neck malignancies are more likely to develop new head and neck tumors in other locations, with the same or different histology. Combinations of two primary malig-nancies are seen in around 3% to 5% of patients with a prior history of cancer, combina-tions of three cancers in about 0.5 percent, and combinations of four malignant tumors in about 0.3 percent of patients with a previous history of cancer [5]. Synchronous head and neck cancers account for 15% of all cases, while metachronous head and neck cancers account for 4%. The median duration from initial malignancy diagnosis to subsequent can-cer occurrence is 31-43 months [5]. As young people with early-stage cancer live longer than those with advanced disease, the prevalence of secondary cancers is higher among them [5]. The cause of numerous head and neck cancers is unknown, but several theories have been proposed, including carcinogen exposure, genetic vulnerability, immunological compromise, and early treatments used to treat primary cancer that result in several sec-ondary tumors [5].
Case Presentation
A 49-year-old male diabetic, hypertensive, non-smoker developed toothache followed by loose teeth in December, 2017. On visiting hospital, during tooth extraction, ulceration was seen at the left gingiva and adjoining floor of mouth and a biopsy was taken, which sug-gested malignancy. Subsequently he underwent wide local excision of the growth at floor of mouth with segmental mandibulectomy and left modified radical neck dissection and right supraomohyoid neck dissection in December 2017. The post operative histopathological report suggested well differentiated squamous cell carcinoma of size 3.2x2.5x1 cm, depth of infiltration 1.5 cm with negative margins and no nodal metastases (pT4aN0M0). Thereafter he received adjuvant radiation by 3D-CRT to 60 Gy in 30 fractions at the rate of 2 Gy per fraction over 6 weeks in 10th January to 20th February, 2018 with concurrent weekly cisplatin chemotherapy. After a disease free interval of nearly 2 years, he again noticed ulceration over right alveolus. He underwent a PET-CT whole body scan which showed a metabolically active soft tissue lesion maybe due to recurrent primary malignancy with few metabolically active small necrotic nodes in bilateral supraclavicular and level VI regions. There was no evidence of metabolically active disease elsewhere. He underwent composite wide local excision, segmental mandibulectomy and right side complete neck dissection in December 2020. Post operative histopathology report suggested moderately differentiated squamous cell carcinoma of size 1x1x0.3 cm, depth of infiltration 0.6 cm with single node positive for metastases and extra nodal extension present staged as rpT1N3bM0 according to the latest AJCC 8th classification. He was planned for adjuvant radiation to the post op site and ipsilateral neck by IMRT technique to 54 Gy in 30 fractions at the rate of 1.8 gy per fraction over 6 weeks with concurrent weekly cisplatin at 40mg/m2 dose from 22nd February to 8th April, 2021. On a follow up MRI scan after 4 months, re-sidual thickening in right buccal mucosa was noted with bony erosion of alveolar part of right maxilla in retromolar trigone. A follow up PET-CT scan of whole body after one month suggested diffuse FDG uptake in right buccal mucosa with FDG avid left supraclavicular lymph node (SUV=3.14) (Figure 1).
Figure 1. PET CT Scan Showing Comparative Images with Post op Changes on 28.01.2021 and Recurrent FDG Avid Areas on 09.08.2021.
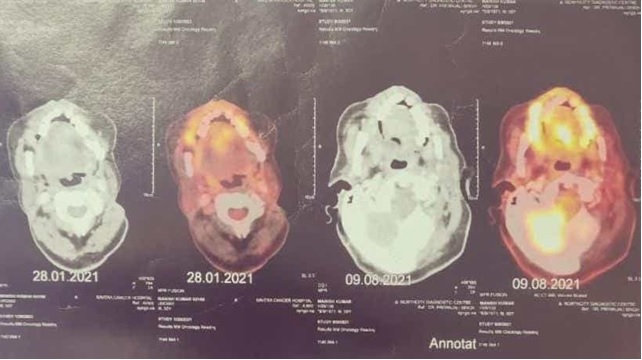
Soft tissue nodular lesion with SUV 19.9 was noted in supraster-nal notch (Figure 2).
Figure 2. FDG Avid Area of Sternal Metastases on 09.08.2021.
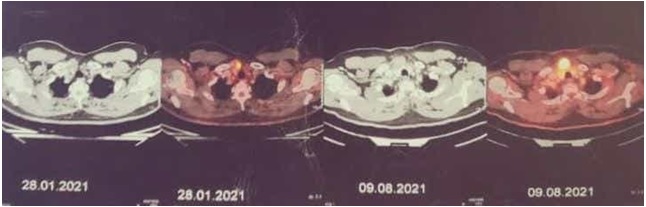
In view of current inoperable status, patient is started on neoadjuvant chemo-therapy with docetaxel, 5-fluorouracil and cisplatin.
Discussion
Patients with squamous cell carcinoma of the head and neck are more prone to acquire a second primary cancer in the upper aerodigestive tract. Patients with recurrent head and neck cancers are usually considered to have poor prognoses [5]. The existence or absence of metastases, as well as the location and size of tumors that may metastasis to lymph nodes in the neck, all affect prognosis [6]. While triple head and neck cancer are uncommon, the risk increases with age, and the consequences of the first tumor on the second primary tumor and vice versa are unknown. The second primary tumor is more aggressive, and synchronous tumors have a far worse prognosis than metachronous malignancies. After head and neck squamous cell carcinoma, second primary malignancy (SPM) is the greatest cause of death in Western literature [1,7,8].
In our case also, the disease-free interval significantly decreased between the first and se-cond and then the second and the third occurrences. Also, the tolerability for the third time treatment was poor and may be attributed to developing resistance to treatment and dete-riorating general condition.
In conclusion, triple head and neck cancer, which is most often seen in the aerodigestive tract, is a very unusual disease with a significant risk of morbidity and death. The frequency rises with age, necessitating a screening programme to obtain an early diagnosis.
References
- Global Cancer Observatory International Agency for Research on Cancer. World Health Organization. Available at: https://gco.iarc.fr/ (Accessed on December 13, 2021)...
- Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries Sung Hyuna, Ferlay Jacques, Siegel Rebecca L., Laversanne Mathieu, Soerjomataram Isabelle, Jemal Ahmedin, Bray Freddie. CA: a cancer journal for clinicians.2021;71(3). CrossRef
- Field cancerization: Definition, epidemiology, risk factors, and outcomes Willenbrink Tyler J., Ruiz Emily S., Cornejo Christine M., Schmults Chrysalyne D., Arron Sarah T., Jambusaria-Pahlajani Anokhi. Journal of the American Academy of Dermatology.2020;83(3). CrossRef
- A genetic explanation of Slaughter's concept of field cancerization: evidence and clinical implications Braakhuis BJ, Tabor MP, Kummer JA, Leemans CR, Brakenhoff RH. Cancer Res.2003;63(8):1727-1730.
- Multiple cancers of the head and neck Heroiu Cataloiu AD, Danciu CE, Popescu CR. Maedica (Bucur).2013;8(1):80-5.
- Synchronous and metachronous head and neck carcinomas Lh Schwartz, M Ozsahin, Gn Zhang, E Touboul, F De Vataire, P Andolenko, J Lacau-Saint-Guily, A Laugier, M Schlienger. Cancer.1994;74(7). CrossRef
- Simultaneous Triple Primary Head and Neck Malignancies: A Rare Case Report Singh Ningombam Jiten, Tripathy Nishikanta, Roy Paromita, Manikantan Kapila, Arun Pattatheyil. Head and Neck Pathology.2016;10(2). CrossRef
- Triple Head and Neck Carcinoma: Case Report and Literature Review I Awad Baraa, Melibari Bashair, Safadi Nabeel, Al-Garni Mohammed, Al-Hakami Hadi Afandi. Cureus.2020;12(2). CrossRef
License

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright
© Asian Pacific Journal of Cancer Care , 2022
Author Details
How to Cite
- Abstract viewed - 0 times
- PDF (FULL TEXT) downloaded - 0 times
- XML downloaded - 0 times